Spatially Fractionated Radiation Therapy
A look at the history, approaches, and new research of spatially fractionated radiation therapy.
In radiation therapy, 3D printing has been investigated to create phantoms and custom patient-specific devices.
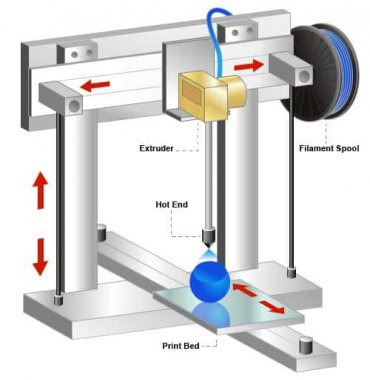
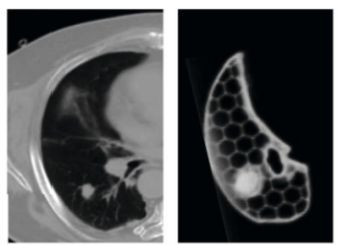
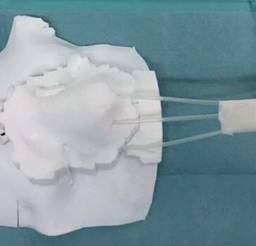
3D printing can also be used in radiation therapy to create patient-specific phantoms for QA based on CT or MR images of the patient. Gear, et. al investigated creating prototypes of 3D printed liquid-fillable liver, spleen, and kidney shells, which resulted in patient-specific phantoms that were durable and able to be reused for multiple SPECT and PET/CT scanning protocols (2).


After working with Radformation as part of an industry cooperative while pursuing her medical physics MS at Hofstra University, Carly now contributes to the AutoContour team as a Clinical Data Analyst. In her free time she enjoys planning game nights with her friends and family.
Related tags: RadOnc News
A look at the history, approaches, and new research of spatially fractionated radiation therapy.
Perspectives from clinical physicists on how COVID-19 has transformed radiation therapy.
Technology and organizations contributing to breast cancer innovation, research, and awareness.
Leave a comment